⏱ 4 Min Read
Your complete guide to preparing for a GP appointment: gynaecology edition
Written by
Eleni Stefanou
Updated on
2 Oct 2023
If you’ve ever felt deflated leaving the GP surgery, this guide is for you. While many GP appointments go smoothly, the reality is that women are up against short session times and the gender pain gap. Read on for our top tips on how to own the room and get what you need from a medical appointment.
Prep like a pro
It’s likely your GP will see between 80-100 patients in a day. Their time is strained, so while they’ll want to show up for you, they are also under pressure to process things quickly. That’s where preparation comes in.
Before your appointment, think through what you want to discuss (usually, it’ll be a combination of symptoms and questions). The next step is to prioritise your ‘talking points’ (imagine planning a meeting agenda at work). This way, if you run out of time, you’ve addressed the most pressing issues first.
Once you’ve written everything down, ask yourself: what do I want the outcome of this appointment to be? It might be reassurance, further investigations (eg a referral, scan or test) or it could be starting a new treatment. Maybe it’s all three.
Now look back at your notes and write them up again, sequencing everything so that your script/bullet points are focused on helping you achieve your goal. Here’s an example:
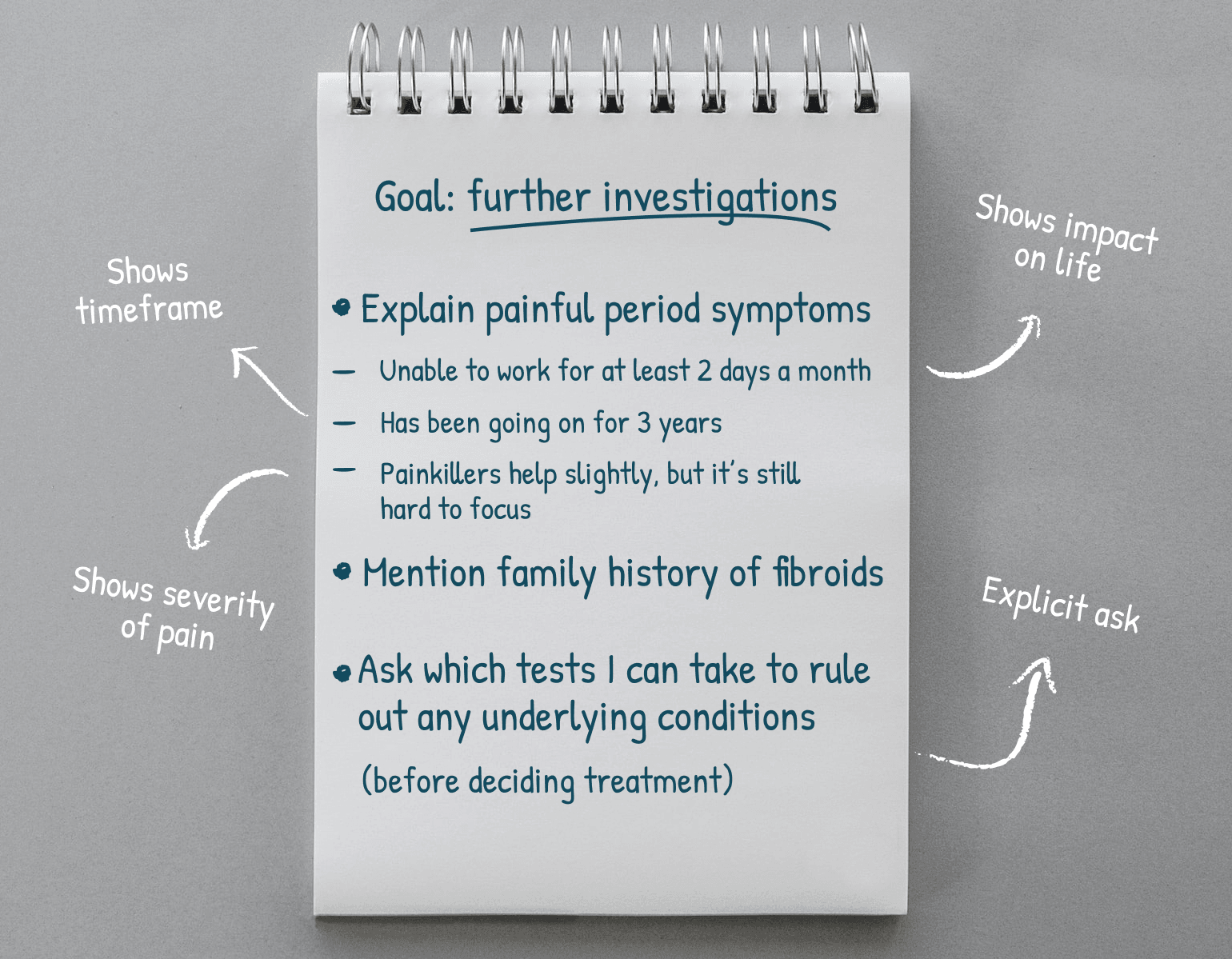
Anticipate questions
Based on the symptoms you’re presenting with, your doctor may ask for further information. For example, they might ask about your last period (when you had it, how many days it lasted). Think about what they’re likely to ask and prepare your answers in advance. This saves time during the appointment and helps your doctor form a clearer clinical picture.
Spend 10-15 minutes researching your health concern online (the NHS is a great place to start and Bloomful’s knowledge hub is your go-to for gynae-specific subjects). Based on your findings, try to anticipate what the doctor might ask you. For example, if you are having heavy periods, the doctor might ask if you experience fatigue, to see if you’re losing so much blood that you could be anaemic. This might not be one of your symptoms, but because you've done your research, you could say: “I don’t feel fatigue, but I do experience spotting between periods and have to change my pads every hour”, signalling to the doctor that your symptoms are worth further investigation.
There’s a high chance your doctor will ask you for timeframes (eg “how long have you been experiencing this symptom for?” or “how long is your average cycle?”), so make sure you have this information ready.
Be prepared to push back
What do you do when the doctor says “painful periods are common, it’s nothing to worry about”? Challenging a medical professional can feel intimidating so try to soften your mind in the moment by leaving room for the possibility that the doctor just wants to reassure you. Serious gynaecological conditions like cancers are rare, so the message they may be trying to send is that there’s unlikely to be cause for concern.
As an advocate for yourself (and women everywhere!), you could respond by saying: “I appreciate many women experience painful periods, however, I read on the NHS website that I should speak to my GP if I experience severe pain. My cramps are so bad that I have to stop working several times a day.”
At that point, the doctor might suggest painkillers to help ease your symptoms. If you think you might have an underlying condition and your goal is to be investigated further, you could say: “While I am open to trying stronger painkillers, I am concerned there may be an underlying condition as I am also experiencing x symptom. I am planning to have children in the future and know that certain conditions can present risks if left untreated. Would it be possible to carry out further investigations?”
If you need clarity on treatment options the doctor is suggesting, don’t be afraid to say: “I understand that there are pros and cons to every treatment. Could you help me compare these treatments?"

Ask someone you trust to come with you
If you’re worried you might freeze in the moment or have trouble advocating for yourself, it might be worth bringing a friend or family member along to the appointment. This isn’t uncommon, so your GP will be used to the experience.
Your companion can give you a morale boost by being there and even step in for you if needed. They can also help you absorb and remember everything the doctor says (two ears are better than one). Take them through your notes in advance and let them know what goal(s) you’ve set for the appointment.
Be honest
If you’re someone who downplays your symptoms or tells themselves you don’t have it as bad as others, make sure you leave this energy outside the examination room. Even if your symptoms aren’t considered severe, it’s important to express how they’re affecting your day-to-day life. Do they cause you anxiety that makes it hard to focus at work or get a good night’s sleep? Are you worried about how your symptoms might affect your fertility? Your doctor will take these factors into consideration when deciding whether to refer you for further investigations, so be honest and share the full picture with them.
Seek out the specialist
When you’re booking your GP appointment with the receptionist, ask them who the best person to speak to about your condition/question is. If they say something along the lines of “all GPs can cover this subject“, you can respond with: “To your knowledge, do any of the doctors specialise or have a keen interest in women’s health?” You still might not get a satisfactory answer, but it’s worth trying.
Get a second opinion
There are complex reasons why gynaecological conditions can take a long time to diagnose. Many symptoms overlap making it hard to determine the underlying cause. Period cramps, for example, can be caused by both endometriosis and non-cancerous growths called fibroids. Some doctors have encountered more cases than others and, as a result, may be more familiar with the nuances of each condition. So if you don’t get answers the first or even second time around, book an appointment with a different GP to see if you can make further progress.
Quick recap
Identify the outcome you want
Organise your talking points
Prepare for likely questions
Take a friend with you for support
Care from the comfort of your home
When was the last time you felt truly heard by a healthcare professional? At Bloomful, our clinicians listen deeply, ask the right questions, and commit to helping you overcome the health hurdles that are holding you back.
